What Happens During a Sleep Apnea Test? A Complete Guide for First-Time Patients
If your doctor has recommended a sleep apnea test, you might be feeling a mix of curiosity and nervousness. What exactly happens during one of these tests? Will you be able to sleep with all those wires attached? And most importantly, what will the results tell you?
Let’s walk through everything you need to know about sleep apnea testing so you can approach your appointment with confidence.
Why Your Doctor Ordered a Sleep Apnea Test
Before we dive into the test itself, it helps to understand why you’re here. Your doctor likely noticed some telltale signs: maybe you’re exhausted despite getting eight hours in bed, your partner complains about your loud snoring, or you’ve been waking up with headaches. These symptoms suggest your breathing might be interrupted during sleep, which is exactly what a sleep apnea test is designed to detect.
The test measures how often your breathing stops or becomes shallow throughout the night, along with dozens of other data points that paint a complete picture of what’s happening while you sleep.
The Two Types of Sleep Apnea Tests
There are actually two main ways to test for sleep apnea, and which one you’ll have depends on your specific situation and your doctor’s recommendation.
In-Lab Sleep Study (Polysomnography)
This is the gold standard for diagnosing sleep apnea. You’ll spend the night at a sleep clinic where trained technicians monitor you throughout the night. It’s the most comprehensive option and can detect a wide range of sleep disorders beyond just sleep apnea.
Home Sleep Apnea Test
This option lets you conduct the test in your own bed. You’ll pick up or receive equipment that you wear overnight, then return it for analysis. Home tests are more convenient and less expensive, but they measure fewer data points than an in-lab study.
Your doctor will recommend the option that makes the most sense for your symptoms and medical history. If your case is straightforward, a home test might be sufficient. If you have other health conditions or more complex symptoms, an in-lab study provides more detailed information.
What to Expect with an In-Lab Sleep Apnea Test
Let’s focus on the in-lab experience, since this is what many people find most intimidating. The reality is far less scary than you might imagine.
Arriving at the Sleep Center
You’ll typically arrive at the sleep center in the evening, usually between 8 and 10 PM. Bring everything you’d normally use for your bedtime routine: comfortable pajamas, toiletries, any medications you take, and maybe a book if you like to read before bed. The goal is to replicate your normal sleep routine as much as possible.
The room itself will surprise you. It’s not a sterile hospital room but more like a hotel room with a comfortable bed, nightstand, and usually a TV. The main difference is the camera and equipment that allows technicians to monitor you from another room.
The Setup Process
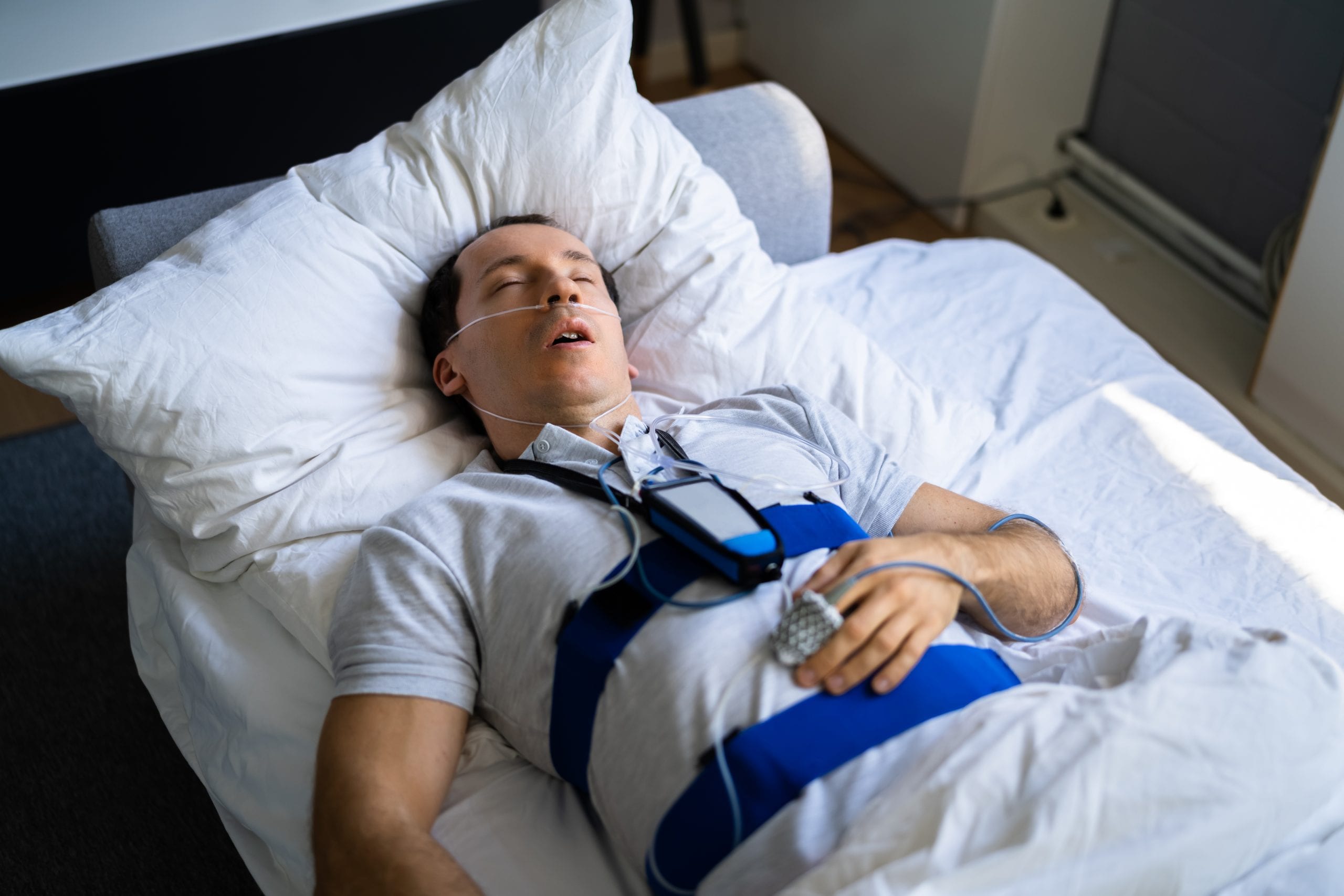
Here’s where things get interesting. A sleep technician will attach various sensors to your body, and yes, there are quite a few of them. Let’s break down what each one does:
On your head and face: Small electrodes get placed on your scalp to measure brain waves, near your eyes to track eye movement, and on your chin to monitor muscle activity. These help determine what stage of sleep you’re in.
On your chest: Sensors measure your heart rate and breathing effort. You’ll also have elastic belts around your chest and abdomen to track breathing movements.
On your legs: Electrodes on your legs detect any movements during sleep, which can indicate certain sleep disorders.
On your finger: A small clip measures your blood oxygen levels throughout the night.
Near your nose and mouth: Sensors track airflow to detect when your breathing stops or becomes shallow.
The technician will also place the wires in a way that allows you to move around and change positions during the night. Everything gets bundled together so you’re not tangled up in individual wires.
Lights Out
Once you’re all set up, you can relax in bed, watch TV, or read until you’re ready to sleep. When you’re ready, you’ll let the technician know through an intercom system, and they’ll turn off the lights. The technician monitors everything from another room and can hear you if you need anything during the night.
I won’t sugarcoat it: sleeping with all these sensors attached feels weird at first. You’re in an unfamiliar place, you’re being watched (though it’s just for medical monitoring), and you’ve got wires all over you. Most people wonder, “How am I supposed to fall asleep like this?”
Here’s the thing: you don’t need to sleep perfectly for the test to work. Even if you sleep less deeply than usual or wake up more often, the technicians will gather enough data to make an accurate diagnosis. They’re used to working with people who don’t sleep their best, and the equipment is sensitive enough to capture what’s needed even from a somewhat restless night.
During the Night
If you need to use the bathroom during the night, just call out or move around and the technician will come help you disconnect temporarily. They’ll reconnect everything when you return to bed.
If you’re someone who usually sleeps less than four or five hours, let the staff know beforehand. They can adjust the testing schedule to match your typical sleep pattern.
Morning Wrap-Up
In the morning, the technician will wake you at a predetermined time (usually around 6 AM) and remove all the sensors. You can shower if you’d like, as some of the adhesive from the electrodes might leave residue in your hair. Then you’re free to go home.
Understanding Your Home Sleep Apnea Test
If you’re doing a home test instead, the process is much simpler. You’ll receive equipment that typically includes a small device that measures breathing, oxygen levels, and heart rate. Some versions are worn on your finger and wrist, while others involve sensors placed on your chest.
The sleep center will provide detailed instructions on how to put everything on before bed. You’ll wear the equipment for one to three nights (depending on what your doctor orders), then return it for analysis. The key advantage is sleeping in your own comfortable bed, though you’ll have less comprehensive monitoring than with an in-lab study.
What Happens Next
After your sleep apnea test, a sleep specialist will analyze all the data collected during the night. This typically takes one to two weeks. They’re looking at how many times your breathing stopped or became shallow per hour (called the Apnea-Hypopnea Index or AHI), your oxygen levels, sleep stages, and other factors.
Your doctor will schedule a follow-up appointment to discuss the results and, if you have sleep apnea, talk about treatment options. The good news is that sleep apnea is very treatable, and most people feel dramatically better once they start treatment.
Tips for a Successful Sleep Apnea Test
Want to make your testing experience go as smoothly as possible? Here are some practical tips:
Avoid caffeine in the afternoon and evening before your test. Don’t take naps on test day. Try to maintain your regular sleep schedule in the days leading up to your test. If you normally use products in your hair, skip them on test day as they can interfere with the scalp electrodes. Bring something that helps you relax, whether that’s a favorite book, calming music, or breathing exercises.
Most importantly, try not to stress about whether you’ll sleep well enough for the test. Remember, the technicians have seen it all, and they’re experts at gathering usable data even when patients don’t sleep perfectly.
Moving Forward
A sleep apnea test might seem daunting, but it’s really just one night (or a few nights at home) that could dramatically improve your quality of life. Poor sleep affects everything from your mood and energy levels to your long-term health. Getting tested is the first step toward finally waking up feeling rested and reclaiming your daytime energy.
If you have questions about your upcoming sleep apnea test, don’t hesitate to call the sleep center beforehand. They’re there to help you feel comfortable and understand the process. You’re taking an important step toward better health, and that’s something to feel good about.